Are you asking yourself, "Am I Pregnant?"
You are not alone! Many women often ponder their pregnancy status in the first couple of weeks after ovulation.
Chances are you won't experience any true pregnancy symptoms until the time when you missed your period, or even a week or a few weeks later than this. It may be even more difficult to determine if you are having signs and symptoms of pregnancy if you don't regularly monitor your menstrual cycle.
There are however, some telltale signs of early pregnancy that many women experience.
Sore or Swollen Breasts
This is often one of the first signs of pregnancy. When you are pregnant, your breasts become excessively sensitive and sore. Even the trickle of the shower head hitting your breasts may be uncomfortable. This sensitivity is due to rising levels of hormones. It may feel somewhat like your breasts feel before your menstrual cycle, only magnified.
Typically breast soreness lasts through the first trimester, and then generally subsides for a time.
Fatigue
The first trimester is typically one filled with fatigue. Feeling tired all the time is absolutely normal, especially given the tremendous work your body is doing to create life! Your body starts producing elevated levels of progesterone during pregnancy, to help prepare the uterus to maintain a pregnancy for nine months. The elevated levels of this hormone can contribute to exhaustion. Fatigue is typically most common during the first and third trimesters, with a break during the second trimester.
Slight Spotting or Implantation Bleeding
Some women will not get their period, but will have some slight spotting or brownish staining early in their pregnancy. If an egg is fertilized, it burrows into the lining of the uterus, usually about six to eight days after fertilization. This may result in a small amount of bleeding referred to as “implantation bleeding.” This is not to be mistaken for actual menstrual bleeding, which is typically heavier and prolonged.
Nausea
Most women will not experience nausea or morning sickness until 2-4 weeks into their pregnancy, however some will start feeling nauseous right away. Morning sickness is truly a “misnomer” as a woman might feel nauseous any time of day. Some will in fact feel ill all day (morning, noon and night!).
Frequent Urination
Most women start having to use the bathroom more frequently shortly after they become pregnant. Typically this is the result of an increased production of blood and fluids in the body. Most women will not experience this symptom until several weeks into their pregnancy, and for some women the need to urinate frequently becomes worse throughout their pregnancy.
Other Early Pregnancy Symptoms
Other early signs of pregnancy reported by a number of women include:
* Menstrual like cramping in the lower abdomen with no bleeding.
* Increased sensitivity to odors.
* Food aversions.
* Elevated body temperature.
* Simply feeling “not quite right.”
Of course, the one almost sure fire way most women find they are pregnant is after they miss their period and take a home pregnancy test. If you are having symptoms of pregnancy and test the first day after you miss your period, keep in mind your test may or may not come back positive at that point.
Depending on the sensitivity of the test and the amount of pregnancy hormone in your body, it may take a few days before you get a positive reading. When you do get a positive test, be sure to contact your healthcare provider to set up your first prenatal visit!
A Basic List of Main Pregnancy Symptoms
Pregnancy Symptoms: Stages of Development
A baby goes through several stages of development, beginning as a fertilized egg. The egg develops into a blastocyst, an embryo, then a fetus.
Fertilization
During each normal menstrual cycle, one egg (ovum) is usually released from one of the ovaries, about 14 days before the next menstrual period. Release of the egg is called ovulation. The egg is swept into the funnel-shaped end of one of the fallopian tubes.
At ovulation, the mucus in the cervix becomes more fluid and more elastic, allowing sperm to enter the uterus rapidly. Within 5 minutes, sperm may move from the vagina, through the cervix into the uterus, and to the funnel-shaped end of a fallopian tube—the usual site of fertilization. The cells lining the fallopian tube facilitate fertilization.
If a sperm penetrates the egg, fertilization results. Tiny hairlike cilia lining the fallopian tube propel the fertilized egg (zygote) through the tube toward the uterus. The cells of the zygote divide repeatedly as the zygote moves down the fallopian tube. The zygote enters the uterus in 3 to 5 days. In the uterus, the cells continue to divide, becoming a hollow ball of cells called a blastocyst. If fertilization does not occur, the egg degenerates and passes through the uterus with the next menstrual period.
If more than one egg is released and fertilized, the pregnancy involves more than one fetus, usually two (twins). Such twins are fraternal. Identical twins result when one fertilized egg separates into two embryos after it has begun to divide.
Development of the Blastocyst
Between 5 and 8 days after fertilization, the blastocyst attaches to the lining of the uterus, usually near the top. This process, called implantation, is completed by day 9 or 10.
The wall of the blastocyst is one cell thick except in one area, where it is three to four cells thick. The inner cells in the thickened area develop into the embryo, and the outer cells burrow into the wall of the uterus and develop into the placenta. The placenta produces several hormones that help maintain the pregnancy. For example, the placenta produces human chorionic gonadotropin, which prevents the ovaries from releasing eggs and stimulates the ovaries to produce estrogen and progesterone continuously. The placenta also carries oxygen and nutrients from mother to fetus and waste materials from fetus to mother.
The wall of the blastocyst becomes the outer layer of membranes (chorion) surrounding the embryo. An inner layer of membranes (amnion) develops by about day 10 to 12, forming the amniotic sac. The amniotic sac fills with a clear liquid (amniotic fluid) and expands to envelop the developing embryo, which floats within it.
As the placenta develops, it extends tiny hairlike projections (villi) into the wall of the uterus. The projections branch and rebranch in a complicated treelike arrangement. This arrangement greatly increases the area of contact between the wall of the uterus and the placenta, so that more nutrients and waste materials can be exchanged. The placenta is fully formed by 18 to 20 weeks but continues to grow throughout pregnancy. At delivery, it weighs about 1 pound.
Development of the Embryo
The next stage in development is the embryo, which develops under the lining of the uterus on one side. This stage is characterized by the formation of most internal organs and external body structures. Organ formation begins about 3 weeks after fertilization, when the embryo is first recognizable as having a human shape. Shortly thereafter, the area that will become the brain and spinal cord (neural tube) begins to develop. The heart and major blood vessels begin to develop by about day 16 or 17. The heart begins to pump fluid through blood vessels by day 20, and the first red blood cells appear the next day. Blood vessels continue to develop in the embryo and placenta.
Almost all organs are completely formed by about 8 weeks after fertilization (which equals 10 weeks of pregnancy). The exceptions are the brain and spinal cord, which continue to mature throughout pregnancy. Most malformations occur during the period when organs are forming. During this period, the embryo is most vulnerable to the effects of drugs, radiation, and viruses. Therefore, a pregnant woman should not be given any live-virus vaccinations or take any drugs during this period unless they are considered essential to protect her health (see Drug Use During Pregnancy).
_______________________________________________________
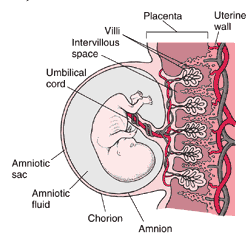
Placenta and Embryo at 8 Weeks
At 8 weeks of pregnancy, the placenta and fetus have been developing for 6 weeks. The placenta forms tiny hairlike projections (villi) that extend into the wall of the uterus. Blood vessels from the embryo, which pass through the umbilical cord to the placenta, develop in the villi. A thin membrane separates the embryo's blood in the villi from the mother's blood that flows through the space surrounding the villi (intervillous space). This arrangement allows materials to be exchanged between the blood of the mother and that of the embryo.
The embryo floats in fluid (amniotic fluid), which is contained in a sac (amniotic sac). The amniotic fluid provides a space in which the embryo can grow freely. The fluid also helps protect the embryo from injury. The amniotic sac is strong and resilient.
__________________________________________________________
Development of the Fetus
At the end of the 8th week after fertilization (10 weeks of pregnancy), the embryo is considered a fetus. During this stage, the structures that have already formed grow and develop. By 12 weeks of pregnancy, the fetus fills the entire uterus. By about 14 weeks, the sex can be identified. Typically, the pregnant woman can feel the fetus moving at about 16 to 20 weeks. Women who have been pregnant before typically feel movements about 2 weeks earlier than women who are pregnant for the first time. By about 23 to 24 weeks, the fetus has a chance of survival outside the uterus.
The lungs continue to mature until near the time of delivery. The brain accumulates new cells throughout pregnancy and the first year of life after birth.
Pregnancy Symptoms: Electronic Fetal Heart Monitoring Part 1
Electronic fetal heart monitoring is done during pregnancy, labor, and delivery to keep track of the heart rate of your baby (fetus) and the strength and duration of the contractions of your uterus. Your baby's heart rate is a good way to tell whether your baby is doing well or may have some problems.
Two types of monitoring, external and internal, can be done.
External monitoring:
You may have external monitoring at different times during your pregnancy, or it may be done during labor.
External monitoring can be done by listening to your baby's heartbeat with a special stethoscope. More often, external monitoring is done using two flat devices (sensors) held in place with elastic belts on your belly. One of these uses reflected sound waves (ultrasound) to keep track of your baby's heart rate; the other measures the duration of your contractions. The sensors are connected to a machine that records the information. Your baby's heartbeat may be heard as a beeping sound or printed out on a chart. The frequency and duration of your uterine contractions are usually printed out on a chart.
External monitoring is used for a nonstress test, which records your baby's heart rate while your baby is moving and not moving. A nonstress test may be combined with a fetal ultrasound to evaluate the amount of your amniotic fluid.
External monitoring is also done for a contraction stress test, which records changes in your baby's heart rate when you have uterine contractions. It may be done to check on your baby's health if your baby does not move enough during a nonstress test. It may help predict whether your baby can handle the stress of labor and vaginal delivery.
Sometimes external monitoring is done remotely (called telemetry), without your needing to be connected by wires to a machine. At some hospitals, the sensors can send the information about your baby's heart rate and your uterine contractions to a remote monitor, usually at a nurse's station. Remote monitoring allows you to walk around freely.
Internal monitoring:
Internal monitoring can be done only after your cervix has dilated to at least 2 centimeters (cm) and your amniotic sac has ruptured. Once started, internal monitoring is done continuously.
For internal monitoring, a sensor is attached to your thigh with a strap. A thin wire (electrode) from the sensor is inserted through your vagina and cervix into your uterus. The electrode is then attached to your baby's scalp. A small tube that measures uterine contractions may be placed in your uterus next to your baby. Your baby's heartbeat may be heard as a beeping sound or printed out on a chart. The strength and timing of your uterine contractions is usually printed out on a chart. Internal monitoring does not use reflected sound waves (ultrasound) for monitoring.
Internal monitoring is more accurate than external monitoring for keeping track of your baby's heart rate and your contractions.
Pregnancy Symptoms: Electronic Fetal Heart Monitoring Part 2
Why It Is Done
External fetal heart monitoring is done to:
Keep track of your baby's heart rate.
Measure how often you have a contraction and how long your contractions last during labor and delivery.
Find out whether you are having preterm labor.
Check on your baby's health if problems are suspected. External fetal heart monitoring will be done during a nonstress test to check your baby's heart rate while at rest and while moving. If your baby does not move during this test, more testing will be needed.
Check on your placenta to make sure that it is giving your baby enough oxygen. A contraction stress test that shows that your baby is not getting enough oxygen helps your doctor make decisions about the safest delivery method. If the test shows that your baby may be in danger, your doctor may recommend starting (inducing) labor early or may talk to you about doing a cesarean section (C-section).
Check your baby's health if your baby has not been growing normally (delayed fetal growth) or if you have diabetes, high blood pressure (hypertension), or are over 41 weeks pregnant.
Internal fetal heart monitoring is done to:
Find out whether the stress of labor is threatening your baby's health.
Measure the strength and duration of your labor contractions.
How To Prepare
You may be asked to eat a meal shortly before having a nonstress test, because digesting food often increases the movement of your baby.
If you are having a contraction stress test, you may be asked to not eat or drink for 4 to 8 hours before the test.
If you smoke, you will be asked to stop smoking for two hours before the external monitoring test because smoking decreases your baby's activity.
Pregnancy Symptoms: Electronic Fetal Heart Monitoring Part 3
How It Is Done
External monitoring can be done any time after 20 weeks of pregnancy. Internal monitoring is used only when you are in labor and your amniotic sac has broken. If internal monitoring is needed and your amniotic sac has not broken, your doctor may break the sac to begin the test. Sometimes a combination of internal and external monitoring is done by measuring your baby's heart rate with an internal sensor and measuring your contractions with an external sensor.
External monitoring
For external monitoring, you will usually lie on a table on your back or left side. Two belts with sensors attached will be placed around your belly. One belt holds the sensor that keeps track of your baby's heart rate, while the other measures the timing and strength of your uterine contractions. Gel may be applied to provide good contact between the heart rate sensors and your skin. The sensors are attached with wires to a recording device that can indicate or print out a record of your baby's heart rate as well as the strength and duration of uterine contractions. The position of the heart rate monitor may be changed periodically to adjust to the movement of your baby.
For a nonstress test, the sensors are placed on your belly. You will be asked to push a button on the machine every time your baby moves or you have a contraction. Your baby's heart rate is recorded and compared to the record of movement or your contractions. This test usually lasts about 30 minutes.
For a contraction stress test, the sensors are placed on your belly. After about 20 minutes of monitoring, uterine contractions are started (induced). To start contractions, you may be instructed to stimulate your nipples or you may be given a medication called oxytocin (Pitocin) in a vein (intravenous, or IV). If oxytocin is given, it will be increased gradually until you have 3 contractions in 10 minutes. Changes in your baby's heart rate in response to your contractions are measured.
Internal monitoring
For internal monitoring, you will usually lie on a table on your back or left side. A thin wire (electrode) will be guided through your vagina and cervix and attached to your baby's scalp. A small tube is also inserted through your vagina to connect a device that monitors the contractions inside your uterus. A belt is placed around your upper leg to keep the monitor in place. The electrode and the tube are attached with wires to a recording device that can indicate or print out a record of your baby's heart rate as well as the strength and duration of your uterine contractions.
How It Feels
Lying on your back (or side) while you are being monitored may be uncomfortable or painful if you are having labor contractions. The belts holding the monitors in place may feel tight.
You may be able to change positions or move around more during internal electronic fetal heart monitoring than during external monitoring.
Placing the internal monitor into your uterus may be mildly uncomfortable.
Risks
You may have a cesarean delivery and not really need it if continuous electronic fetal heart monitoring shows that your baby is in distress when he or she is actually healthy.
If the machine is having technical problems, the machine may show that your baby is healthy when he or she is in distress. This is rare.
There is a slight risk of infection for your baby when internal monitoring is done.
Pregnancy Symptoms: Electronic Fetal Heart Monitoring Part 4
Results
Electronic fetal heart monitoring is done during pregnancy, labor, and delivery to keep track of the heart rate of your baby (fetus) and the strength and duration of the contractions of your uterus. The results of electronic fetal heart monitoring are usually available immediately.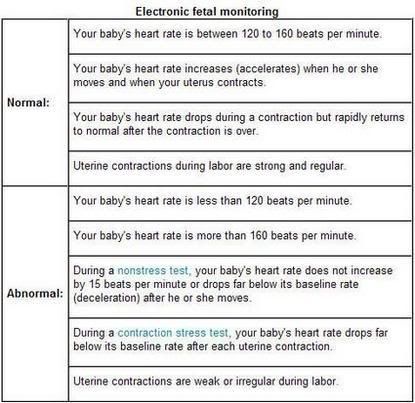
What Affects the Test
Reasons you may not be able to have the test or why the results may not be helpful include:
Smoking cigarettes or using other tobacco products and drinking or eating large amounts of caffeine (such as from several cups of strong coffee), which can falsely raise your baby's heart rate.
Extra noises such as your heartbeat or your stomach rumbling.
Your baby is sleeping during a nonstress test.
Problems with the placement of the external monitoring device. These problems may include:
*Your baby is moving a lot during the test.
*You are pregnant with more than one baby, such as twins or triplets.
*You are overweight.
What To Think About
Not everyone feels the same about fetal monitoring.
Some mothers think that fetal heart monitoring is not needed and interferes with the natural birthing process.
Other mothers think that fetal heart monitoring is reassuring. This may be true if they had problems with earlier pregnancies.
Fetal monitoring cannot predict every type of problem, such as birth defects. Normal fetal heart monitoring test results do not mean that your baby is healthy.
Continuous monitoring during labor is more likely to be useful for high-risk pregnancies.
Intermittent fetal heart monitoring during labor is as effective as continuous monitoring in low-risk pregnancies.
If your baby appears to be having problems, sometimes a blood sample is taken from a small blood vessel (capillary) in his or her scalp. The blood sample can help determine if your baby is receiving enough oxygen.
Your baby may move more if you eat or drink juice before having a nonstress test. This may make the test results more useful.
Sometimes other methods (such as ringing a bell near the uterus) are used to cause changes in your baby's heart rate.
External fetal heart monitoring is used during other tests of fetal health, such as a nonstress test, contraction stress test, and biophysical profile.
Pregnancy Symptoms: Ultrasound Techniques
No ionizing radiation is involved.
Transabdominal ultrasound: A jelly is put on the abdomen, and a hand–held sound–wave wand is moved around to look at the internal structures. The woman’s bladder must be full to help transmit the sound waves, so she may be asked to drink two to three glasses of water starting an hour before the test. This method works best later in pregnancy when the fetus is well developed. The doctor may have a scan performed during the first trimester to make sure the pregnancy is in the uterus and not outside it (ectopic pregnancy) and to assess the woman’s risk for having a miscarriage. The scan can also tell if more than one fetus is developing. During the remainder of the pregnancy, scans may be used to look for problems, assess the age and development of the fetus, check out its position, and, by 17 weeks, determine the sex. There is no risk to the woman or her developing fetus with ultrasound, and it is not uncomfortable. Ultrasounds help doctors establish the due date. Due dates can now be predicted within two to four days if the ultrasound is performed early enough.
Endovaginal or transvaginal ultrasound: A long, thin, sound–wave wand is covered with a condom and put inside the vagina. This type of ultrasound is usually performed early in pregnancy to make sure that the embryo or fetus is inside the uterus where it belongs. This type of ultrasound also gives more detail, for instance, about the structure of the woman’s cervix and the early embryonic anatomy.
Targeted Ultrasound Tests: A targeted or level II ultrasound exam provides a detailed assessment of fetal anatomy. It is recommended if there are concerns for fetal problems based on other tests or history.
Nuchal Fold Translucency Tests: A non–invasive screening for genetic defects. A certified ultrasound technologist measures the fold at the back of the neck. Measurements are then formulated to calculate the risk factor for certain birth defects. It is usually done at 10–14 weeks gestation and offered with a blood test that also screens for birth defects.
Pregnancy Symptoms: Ultrasound
A pregnancy ultrasound is a method of seeing the fetus and female pelvic organs during pregnancy. The ultrasound machine sends out high-frequency sound waves. These waves bounce off body structures to create a picture.
How the test is performed:
You will lie down for the procedure. A clear, water-based conducting gel will be applied to your skin over your abdomen and pelvis. The gel helps transmit sound waves. A hand-held probe is then moved over the area.
Another method is performed with the probe placed in the vagina of the patient (transvaginal ultrasound scanning). This technique often complements conventional ultrasound techniques by providing better detail. Consult your health care provider to determine which technique is most appropriate for you.
How to prepare for the test:
A full bladder is necessary to get a good picture. Therefore, you may be asked to drink 2 to 3 glasses of liquid an hour before the test. You should not urinate before the procedure.
How the test will feel:
There may be some discomfort from pressure on the full bladder. The conducting gel may feel slightly cold and wet. You will not feel the ultrasound waves.
Why the test is performed:
Some physicians order an ultrasound when an abnormality is suspected, while others advocate screening ultrasounds. You should consult your health care provider to determine the most appropriate scanning schedule for you.
Scans may be performed in the first trimester to:
Confirm a normal pregnancy
Assess the baby's age
Rule out abnormalities, such as ectopic pregnancies or potential for miscarriage
Assess the baby's heart
See if there are multiple pregnancies
Identify abnormalities of the placenta, uterus, and other pelvic structures
Scans may also be obtained in the second and third trimesters to:
Assess the baby's age, growth, position, and sometimes gender
Identify any developmental problems
Rule out multiple pregnancies
Evaluate the placenta, amniotic fluid, and remaining structures of the pelvis
Some centers are now performing a scan at around 13-14 weeks of pregnancy to look for risks for Down Syndrome (which causes mental retardation) or other developmental abnormalities in the fetus.
The total number of scans will vary depending on whether a previous scan or blood tests have detected abnormalities that require follow-up assessment.
Normal Values:
The fetus and associated pelvic structures are normal in appearance and appropriate for the gestational age.
What abnormal results mean:
Abnormal ultrasound results may be due to some of the following conditions:
Ectopic pregnancy
Multiple pregnancies
Fetal death
Abnormalities of fetal position
Congenital malformations
Amniotic fluid problems, including oligohydramnios (not enough fluid) and polyhydramnios (too much fluid)
Placental abnormalities, including placenta previa and placental abruption
Intrauterine growth retardation
Tumors of pregnancy, including gestational trophoblastic disease
Additional abnormalities of the ovaries, uterus, and remaining pelvic structures
What the risks are:
There is no documented effect on patients and their fetuses with the use of current ultrasound techniques. No ionizing radiation is involved.
Pregnancy Symptoms: Questions To Ask The Doctor
Questions to Ask the Doctor:
Am I at risk for genetic diseases?
How much weight should I gain?
Am I gaining weight too fast?
How should I alter my diet (especially if a vegetarian or a vegan)?
What tests should I have and when should I schedule them?
Am I a high–risk patient?
What is my risk for cesarean birth?
What exercises are safe?
What vaccinations should I have?
What medications may I take?
May we develop a birth plan?
Should I hire a doula?
Will I be allowed to have keepsake ultrasound pictures?
Pregnancy Symptoms: Seeking Medical Care
If a woman suspects that she is pregnant or has a positive home pregnancy test, she should make an appointment with a health care provider, which could be a doctor, an obstetrician (women's health specialist), a midwife, or a nurse practitioner. Early care (prenatal care) is essential for a healthy pregnancy.
A woman who is pregnant should call her health care provider if any of the following conditions develop:
Labor or rupture of membranes (leaking fluid)
Abdominal or vaginal pain
Bright red vaginal bleeding
Vomiting more than three times a day or vomiting blood
Severely elevated blood pressure (above 140/90)
Sudden and rapid weight gain
Severe headache or changes in vision
Severe leg or chest pain
Seek care in a hospital's emergency department if pregnant and experiencing any of these conditions:
Fainting
Vaginal bleeding through more than one pad per hour
Having severe pain in the abdomen or shoulder or the sensation of being about to pass out
Passing pink, gray, or white material from the vagina that does not look like a blood clot (The woman who is pregnant should take the material to the hospital.)
Having a bloody discharge or gush of water from the vagina late in pregnancy (The woman who is pregnant may be going into labor.)
Having a seizure but without a history of epilepsy (This may indicate eclampsia, a complication of pregnancy.)
Having an injury, such as a fall, a blow to the stomach or pelvis, or a car accident
Lower abdominal pain late in pregnancy may be labor pains, which are contractions of the uterus. The woman may try to drink a quart of water, lie on her side, and see if the symptoms resolve over two hours. If the symptoms do not resolve, she should see a doctor.
Pregnancy Symptoms: Implantation Bleeding
Up to 25 percent of pregnant women have light vaginal bleeding, or spotting, during the first trimester. In most cases, spotting is not a sign of a problem. Light bleeding in the first trimester is often caused by the implantation of the fertilized egg in the wall of the uterus. This implantation bleeding usually happens 10 days or so after conception. Implantation bleeding is usually lighter and more irregular than a menstrual period. But any vaginal bleeding during pregnancy or a suspected pregnancy should be taken seriously. If you are pregnant or think you are pregnant, you should always call your doctor if have any bleeding. He or She will be able to figure out if it is a sign of a problem.
Sometimes bleeding in early pregnancy can signal trouble. Call the doctor immediately if you have:
heavy bleeding
bleeding with cramping, pain, fever or chills
bleeding that lasts more than 24 hours
Other common causes of vaginal bleeding in early pregnancy include:
Changes in the cervix: During pregnancy, there is more blood flowing to the cervix. So it is more likely to bleed. Sexual intercourse during pregnancy can sometimes cause a small amount of vaginal bleeding. Also, many women have spotting after a pelvic exam.
Miscarriage: Vaginal bleeding in the first trimester is sometimes a sign of a miscarriage.
Ectopic pregnancy: Vaginal bleeding, that often occurs along with some abdominal pain can be the sign of an ectopic pregnancy. An ectopic pregnancy occurs when the fertilized egg implants outside of the uterus, often in the fallopian tube. This is a serious condition that needs immediate attention. Ectopic pregnancies can not produce a healthy baby. Plus, untreated ectopic pregnancies can seriously harm or kill the mother.
Pregnancy Symptoms: Pregnancy Tests
How do pregnancy tests work?
Pregnancy tests look for a special hormone in the urine or blood that is only there when a woman is pregnant. This hormone, human chorionic gonadotropin (hCG), can also be called the pregnancy hormone. The pregnancy hormone, hCG, is made in your body when a fertilized egg implants in the uterus. This usually happens about 6 days after conception. But studies show that the embryo doesn't implant until later in some women. The amount of hCG increases drastically with each passing day you are pregnant. Many home pregnancy tests claim they can tell if you're pregnant on the day you expect your period. But a recent study shows that most don't give accurate results this early in pregnancy. Waiting one week after a missed period will usually give a more accurate answer.
What's the difference between pregnancy tests that check urine and those that test blood?
There are two types of pregnancy tests. One tests the blood for the pregnancy hormone, hCG. The other checks the urine for this hormone. You can do a urine test at home with a home pregnancy test. You need to see a doctor to have blood tests. These days, most women first use home pregnancy tests (HPT) to find out if they are pregnant. HPTs are inexpensive, private, and easy to use. Urine tests will be able to tell if you're pregnant about 2 weeks after ovulation. Some more sensitive urine tests claim that they can tell if you are pregnant as early as one day after a missed period. If a HPT says you are pregnant, you should call your doctor right away. You doctor can use a more sensitive test along with a pelvic exam to tell for sure if you're pregnant. Seeing your doctor early on in your pregnancy will help you and your baby stay healthy.
Doctors use two types of blood tests to check for pregnancy. Blood tests can pick up hCG earlier in a pregnancy than urine tests can. Blood tests can tell if you are pregnant about 6 to 8 days after you ovulate (or release an egg from an ovary). A quantitative blood test (or the beta hCG test) measures the exact amount of hCG in your blood. So it can find even tiny amounts of hCG. This makes it very accurate. Qualitative hCG blood tests just check to see if the pregnancy hormone is present or not. So it gives a yes or no answer. The qualitative hCG blood test is about as accurate as a urine test.
How accurate are home pregnancy tests?
Home pregnancy tests (HPTs) can be quite accurate. But the accuracy depends on many things.
These include:
How you use them - Be sure to follow the directions and check the expiration date.
When you use them - The amount of hCG or pregnancy hormone in your urine increases with time. So, the earlier after a missed period you take the test the harder it is to spot the hCG. If you wait one week after a missed period to test, you are more apt to have an accurate result. Also, testing your urine first thing in the morning may boost the accuracy.
Who uses them - The amount of hCG in the urine is different for every pregnant woman. So, some women will have accurate results on the day of the missed period while others will need to wait longer.
The brand of test - Some home pregnancy tests are more sensitive than others. So, some tests are better than others at spotting hCG early on.
How soon after a missed period can I take a home pregnancy test and get accurate results?
If you can wait one week after your missed period, most home pregnancy tests will give you an accurate answer. Ask your doctor for a more sensitive test if you need to know earlier.
When a home pregnancy test will give an accurate result depends on many things. These include:
How long it takes for the fertilized egg to implant in the uterus after ovulation - Pregnancy tests look for the hormone human chorionic gonadotropin (hCG) that is only produced once the fertilized egg has implanted in the uterine wall. In most cases, this happens about 6 days after conception. But studies show that in up to 10 percent of women, the embryo doesn't implant until much later, after the first day of the missed period. So, home pregnancy tests will be accurate as soon as one day after a missed period for some women but not for others.
How you use them - Be sure to follow the directions and check the expiration date.
When you use them - The amount of hCG in a pregnant woman's urine increases with time. So, the earlier after a missed period you take a HPT, the harder it is to spot the hCG. If you wait one week after a missed period to test, you are more apt to have an accurate result. Also, testing your urine first thing in the morning may boost the accuracy.
Who uses them - The amount of hCG in the urine at different points in early pregnancy is different for every woman. So, some women will have accurate results on the day of the missed period while others will need to wait longer.
The brand of test - Some home pregnancy tests are more sensitive than others. So, some tests are better than others at spotting hCG early on.
I got a negative result on a home pregnancy test. Might I still be pregnant?
Yes. So, most HPTs suggest women take the test again in a few days or a week. Every woman ovulates at different times in her menstrual cycle. Plus, embryos implant in the uterus at different times. So, the accuracy of HPT results varies from woman to woman. Other things can also affect the accuracy.
Sometimes women get false negative results (when the test says you are not pregnant and you are) when they test too early in the pregnancy. Other times, problems with the pregnancy can affect the amount of hCG in the urine.
If your HPT is negative, test yourself again in a few days or 1 week. If you keep getting a negative result but think you are pregnant, talk with your doctor right away.
Can anything interfere with home pregnancy test results?
Most medicines, over-the-counter and prescription, including birth control pills and antibiotics, should not affect the results of a home pregnancy test. Only medicines that have the pregnancy hormone hCG in them can give a false positive test result. A false positive is when a test says you are pregnant when you're not.
Sometimes medicines containing hCG are used to treat infertility (not being able to get pregnant). Alcohol and illegal drugs do not affect HPT results. But women who may become pregnant should not use these substances.
Pregnancy Symptoms: Pregnancy Overview
Pregnancy occurs when an egg is fertilized by a sperm, grows inside a woman's uterus (womb), and develops into a baby. In humans, this process takes about 264 days, but the obstetrician will date from the last menstrual period or 280 days (40 weeks).
The doctor will use certain terms in discussing a woman’s pregnancy. Some of the following definitions are useful:
Intra–uterine pregnancy: A normal pregnancy occurs when a fertilized egg is implanted in the uterus (womb) and an embryo grows.
Embryo: The term used for the developing fertilized egg during the first 12 weeks of pregnancy.
Fetus: The term used for the developing embryo after 12 weeks of gestation.
Beta human chorionic gonadotropin (also called beta–hCG): This hormone is secreted by the placenta and can be measured to determine the presence and progression of the pregnancy. Urine or blood can be tested for its presence, and it is the hormone measured by a home pregnancy test. A positive result means a woman is pregnant; however, this test result can stay positive for several weeks after delivering a baby or after a miscarriage.
Trimester: The length of time of a pregnancy is divided into three sections called trimesters (about three months each). Each trimester has particular events and developmental markers. For instance, the first trimester builds the foundation of the different organ systems.
Estimated date of delivery (EDD): The delivery date is estimated by counting forward 280 days from the first day of the woman’s last period. It is also called the estimated date of confinement (EDC).
The woman who is pregnant and her doctor will monitor the pregnancy either to prevent certain conditions from developing or to treat those conditions early. These conditions include the following:
High–risk pregnancy: If a woman is considered to be likely to have complications during pregnancy, the pregnancy may be termed high risk. Examples include pregnancies in women with diabetes and those with high blood pressure. Age–related complications can occur in women such as teenagers, women who are over the age of 35, or women who have been treated for infertility or with pregnancies from the use of assisted reproductive technologies.
Ectopic pregnancy: This is a pregnancy in which the egg implants somewhere other than the uterus. This can be life threatening. Ectopic pregnancy must be diagnosed early to avoid damage to the Fallopian tubes and to prevent serious illness or death. It is also called tubal pregnancy (if the egg implants in the Fallopian tubes) or extra–uterine pregnancy.
Cervical Incompetence or Preterm Labor: This is a condition in which the cervix begins to dilate (widen) and efface (thin) before the pregnancy has reached term. Cervical incompetence can be a cause of miscarriage and preterm birth in the second and third trimesters.
Preeclampsia/eclampsia: Preeclampsia is a systemic disease that can affect various organ systems. Vascular effects cause the blood pressure to rise in the woman who is pregnant, changes in kidney function, swelling throughout the body, and alterations in blood chemistry and nerve reflexes. If left untreated, preeclampsia can lead to eclampsia, a serious illness that causes seizures, coma, and even death.
Multiple Gestation (for example twins, triplets): Preterm birth is twice as likely in twin pregnancies as in singleton pregnancies. The percentage of preterm birth is even greater for triplet pregnancies and quadruplet pregnancies. Preeclampsia also occurs three to five times more frequently with multiple gestation.